A study by RHA scientists Kristi MacDonald and Mara Tippett, “Reducing public exposure to common, harmful well water contaminants through targeted outreach to highly susceptible neighborhoods as a method of increasing likelihood of testing and treatment of water from private wells,” was recently completed. The study was funded by New Jersey Water Resources Research Institute (NJWRRI), Rutgers University. The study was recently published in the international peer-reviewed journal Water and Health – access the article here.
The study is summarized here and a link to the full report manuscript is below.
Executive Summary:
- While public water is required by state and federal law to be tested by water purveyors for a variety of contaminants, private well owners are responsible for testing and treating their own water.
- In the Upper Raritan region (WMA8) of New Jersey, 80% of the drinking water comes from private wells yet only a small percentage of well owners test their wells annually and many never test at all for common and potentially harmful groundwater contaminants.
- Finding effective ways to inform residents of the risks associated with their private well drinking water and promoting action to test and treat water for common contaminants is a challenge faced by agencies concerned with public health at the federal, state, and local level.
- In this study, several hypotheses were tested related to perceived risk and the health action of testing and treating well water that may vary with proximity and type of contaminant. Insights into whether a spatial model for predicting private wells at risk for contamination was explored based on rate of wells exceeding drinking water standards if a neighbor’s well exceeded as compared to rate of wells exceeding in the general population of a region.
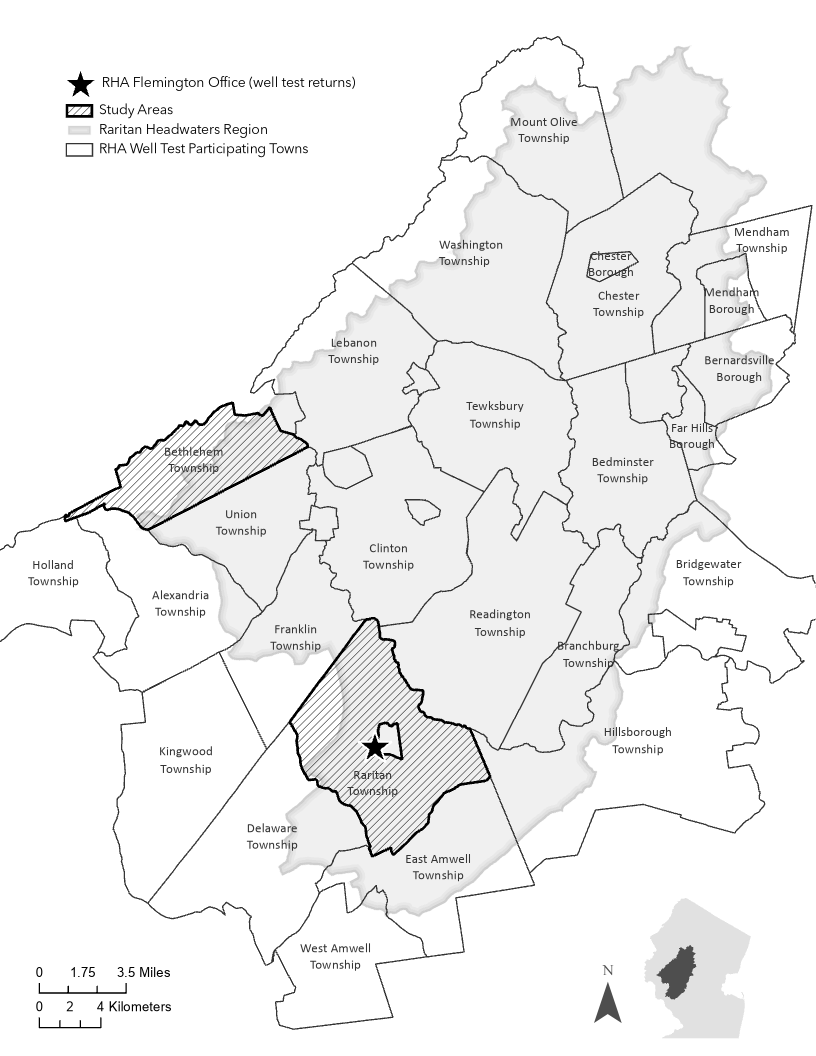
- Data from the Raritan Headwaters Association (RHA) Well Test Program (www.testmywell.org) collected from Raritan and Bethlehem townships in Hunterdon Co., New Jersey, USA were used to identify private wells that exceeded state and federal drinking water standards for 5 common, harmful contaminants of groundwater in our region: arsenic, radionuclides (radon and Gross Alpha), E. coli, and nitrates. Residents within 1,000 feet of the well address (n=2106) received notification that a nearby well had a specific contaminant(s) above the Maximum Contaminant Level (MCL) and a random sample of residents (n=491) received a letter that provided information on the regional rates of exceedances of the MCLs for the 5 contaminants. All were encouraged to test their well water through RHA’s discounted well testing program.
- Overall, 10% (n=258) of people receiving letters responded and of these, 71% (n=183) tested their wells. Individuals who received specific letters that a contaminant in a neighbor’s well had exceeded the MCL were more likely to test their well than were individuals who received a general letter about common contaminants in the region. Of those receiving letters regarding specific contaminant(s) in a local well, 8.2% (n=172) tested their well whereas of those receiving a general letter only 2.2% (n=11) tested. The likelihood of testing did not differ between townships or among the type of contaminants. Outreach that reports more localized, specific information on contaminants in well water results in an increased chance of testing as compared to more regional and generalized contaminant information.
- Of individuals who tested, 29% detected a contaminant above the MCL. A telephone survey of these participants was conducted to explore whether residents treated the water. Of the 22 survey respondents, 36% (n=8) treated their well water as a result of their test exceeding the drinking water standard. However, very few respondents (5%, n=1) reported switching their water source as a result of testing. Prior to testing, 36% (n=8) drank bottled water, 23% (n=5) drank unfiltered well water, and the rest drank filtered well water. Ninety-five percent of participants did not switch their water source after learning that their well exceeded the drinking water standard for one or more contaminants. Most respondents indicated that testing increased their confidence in their well water, even if they learned their water was exceeding the drinking water standard for a contaminant. In addition, 2 nearly all respondents planned to test their well again in the future. These results indicate that a large portion of well test participants are not treating contaminants that exceed the drinking water standards. In addition, it appears that initial testing and detection of exceedances promotes future testing.
- The likelihood of exceeding the drinking water standard for at least one of the 5 contaminants from a sample of 189 individual tests was 18% (n=34) for those receiving a letter about a specific exceedance locally whereas the likelihood of exceeding the MCL for one of those 5 contaminants in the two municipalities between 2012 and 2018 (n=1607) was 5% (n=86). None of the towns showed a higher likelihood for exceeding the MCL for arsenic or Gross Alpha if a neighbor exceeded for those contaminants, respectively. However, for Bethlehem Township and both towns combined, E. coli and nitrate had a higher likelihood of exceeding the MCL if a neighbor’s well exceeded. Furthermore, for towns combined but not individual townships, radon had a higher likelihood of exceeding federal guidelines if a neighbor’s well exceeded as compared to the combined township data from 2012-2018. This indicates that in some but not all cases, the likelihood of exceeding may be predicted to some degree based on existing well test data and outreach to residences may be targeted.
- While letters about local contaminants does help target residents and boost testing to some extent, more research is needed on how to get the majority of residents to respond with health actions of testing and treating their private well water. Further studies into how the originating source of outreach information impacts perceived reliability of data are needed. In addition, developing predictive models of likelihood of exceedances for contaminants will help to make outreach more efficient and successful in reaching those most at risk.



